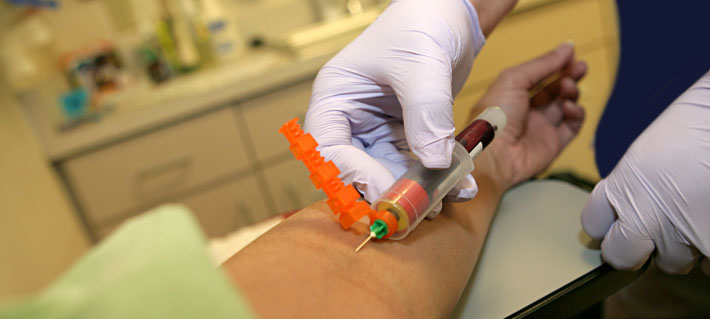
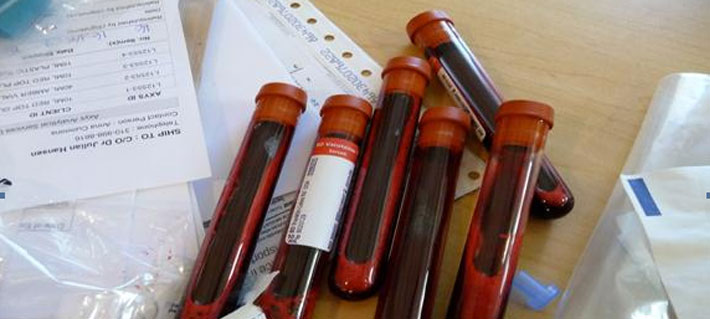
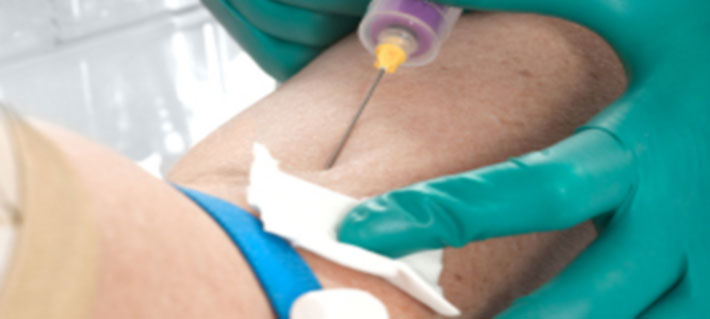
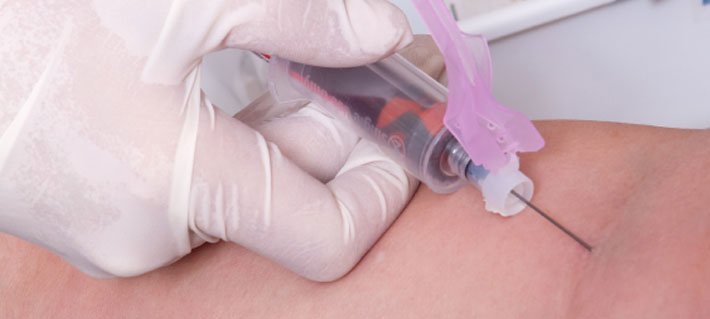
Welcome to Contra Costa Medical Career College
Comprehensive Basic and Advanced Phlebotomy On-Line for experienced health care providers
Are you already working in the health-care field? Have you done at least 50 venipunctures, and at least 10 skin punctures while working with real patients (not practicing or being trained in a program of any kind) in the last 5 years? Have you always wanted to become certified as a Phlebotomy Technician (CPT1)? If the answer is YES, then Contra Costa Medical Career College’s Online Phlebotomy Technician Courses can help.
Now more than ever, employers such as hospitals, doctor’s offices, out-patient labs and nursing homes require medical health-care workers to perform blood draws. The state of California and many employers all over the country require employees who draw blood in the laboratory setting to be certified as a Phlebotomy Technician, you cannot work as a "Phlebotomist" in California without it.
Contra Costa Medical Career College recognizes the need for accelerated training for those already in the medical profession and who may be skilled in the art of drawing blood but lack certification. Physicians, nurses, RN’s, LPN’s, LVN’s and Medical Technologists sometimes require extra training with regard to their phlebotomy skills. They can now certify via taking the Contra Costa Medical Career College’s online phlebotomy certification courses.
What are the course goals?
The course provides an overall review of the most current phlebotomy practices and procedures with an emphasis on the most important competencies. A large variety of application exercises, videos, quizzes, and exams give plenty of practice taking tests and will ensure successfully completion of any California CDPH-LFS Approved National Phlebotomy Exams.
Who should take this course?
Individuals with at least 6 months experience
Seeking to obtain California State certification as a CPTI are required to complete the Advanced Course only. We recommend however that both courses are completed. The National exam required by the State of California includes information covered in both the Comprehensive Basic and Advanced Didactic courses. No externship is required. However, these individuals will be required to provide a completed California experience document signed by a Laboratory Director/MD, DO, CLB. Experience must involve on the job experience on real patients (not during a training program of any kind).
Individuals with less than 6 months experience
Seeking to obtain California State certification as a CPTI are required to complete both the Comprehensive Basic Didactic and the Advanced Didactic courses. No externship is required. However, these individuals will be required to provide a completed California experience document signed by a Laboratory Director/MD, DO, CLB. Experience must involve on the job experience on real patients (not during a training program of any kind). To the extent that the Comprehensive Basic Course provides preparation for the Advanced Course it is recommended that all persons qualifying on the basis of experience complete both Comprehensive Basic and Advanced courses and in that order.
Individuals with No Experience: CAN NOT take our online courses
These courses do not qualify you to become certified as a Limited Phlebotomy Technician.
Students without phlebotomy experience, who wish to become CPT1 certified in the state of California must participate in a CDPH-LFS approved, FULL program with externship. A full program is a program that combines basic didactic, advanced didactic and at least 40 hour externship experience.
Licensed and non licensed health care professionals
Including LVN's, CNA's, EMT's, PCT's and others may expand their scope of practice by obtaining certification as CPTI.
Individuals preparing to sit for National Certifying Exams
Most national certifying agencies accept California Approved Didactic training as partial fulfillment of prerequisites for taking their phlebotomy certifying exam. Please contact the National Certification agency directly with questions you may have. You will find a list of California State approved testing agencies on the CDHS-LFS website.
California Residents
DO NOT take the online courses if your goal is to become licensed in the State of California AND:
- You have no experience
- If your experience was longer than 5 years ago.
When is it offered and how?
It’s online. Anytime, anywhere, in the convenience of your own home or office! No out of pocket expenses or travel costs
Tuition and fees:
- Comprehensive Basic Phlebotomy and Advanced Phlebotomy Online: $698.00
- Advanced Phlebotomy Online: $399.00
- Note: Course price does not include required textbook.
"Phlebotomy Essentials 7th Edition", Ruth E. McCall and Cathleen M. Tankersley (Lippincott Williams & Wilkins) ISBN-13: 978-1-4963-8707-3. The book is approximately $55.00. A link to purchase the book is available when you sign up for the course. You will need the textbook to complete the course successfully.
Check specific laws and regulations in the State in which you reside. Laws differ from state to state.
Phlebotomy Certification
California is often a pioneer in healthcare industry workplace regulations. Those with blood drawing responsibilities in the state of California must now first become a Certified Phlebotomist. This requirement went into effect on April 9, 2003, with the exception for experienced phlebotomists who were at that time already working in the field. They had up to three years to meet the new standards, which means by 2006 all phlebotomists in California had to be certified in order to practice the skill.
Browser Compatibility
We are constantly updating our compatibility matrix. Please contact us if you have any issues with this website.